Interventional pain management at Agape will typically consist of minimally invasive procedures to reduce pain. At Agape Pain Management of Las Cruces, we utilize a multidisciplinary approach to managing joint and back pain. One of these approaches is therapeutic injections. These Injection procedures are performed by specially trained clinicians and can be done in our office under fluoroscopy guidance. In addition, your interventionist works closely with other specialists such as physical therapists, chiropractors, and surgeons to manage pain and improve function.
Epidural steroid injection
Epidural steroid injections (ESI) involve injecting medications along the nerve roots attached to the spinal column. The type of pain treated with this type of injection occurs when one of the spinal cord nerve roots becomes compressed and irritated. This compressed nerve root can cause neck and/or back pain accompanied by numbness, tingling and occasionally extremity weakness. This injection is a safe procedure performed by a thoroughly trained and qualified physician utilizing fluoroscopic guidance. Often, this injection can help identify the specific source of pain and aid in the diagnosis. Thus, the procedure can be both diagnostic and therapeutic, assisting surgeons in identifying the source of pain while still providing you with relief.
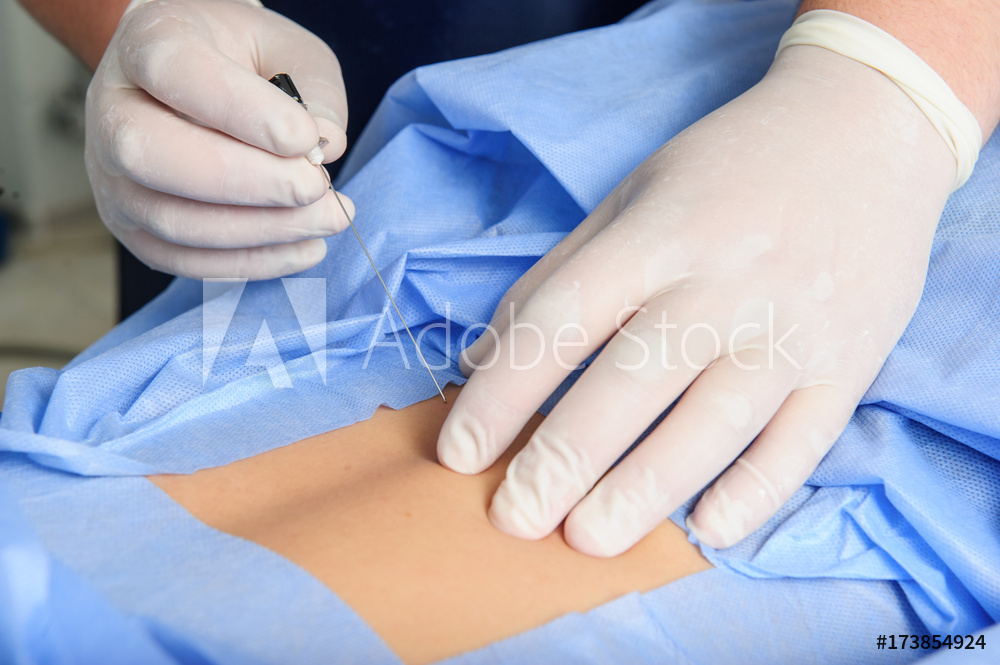
Facet joint injection
Just as with the Epidural Steroid Injection, a Facet joint injection can also be therapeutic and diagnostic. At each vertebral level, a pair of facet joints allow movement of the spine and provide stability. However, facet joint inflammation is usually the cause of significant back pain while sitting. Therefore, an anesthetic agent and a steroid are injected into the facet joint space to reduce inflammation and decrease pain. For maximum benefit, These injections are typically done in combination with physical therapy.
Medial Branch Blocks
Medial branch blocks are tools used to help diagnose and relieve back pain from degenerative and painful facet joints. The medial branch is a nerve that relays pain signals from the facet joint to the spinal cord. A medial branch is located above and below each joint, which conveys pain signals for every joint. For this procedure, the local anesthetic is injected over two medial branches, blocking the pain signals from a facet joint.
Radiofrequency Ablation
After a Medial Branch Block procedure or a Facet Joint Injection has been performed, the exact source of the pain should be identified. Diagnosis allows for radiofrequency ablation (RFA) to be performed on the same nerve roots. Radiofrequency waves treat the specific nerves causing the pain using heat, minimizing the transmission of pain signals to the brain. Therefore, it can provide longer-lasting relief for chronic pain, especially in the back and neck. This RFA procedure is safe and is performed by a fully-trained and qualified clinician in our office. The procedure will usually take 20 minutes or less. Although the results from RFA vary from each individual, after one week, most people typically feel less pain than before their procedure. In addition, most people can expect overall healing time to last four weeks due to the residual effects of the procedure and muscle spasms. The length of pain relief from this procedure varies from person to person but usually lasts from 6 to 12 months.
Sacroiliac Joint Injection
Sacroiliac joint (SI joint) dysfunction is a well-known diagnosis. The sacroiliac joints are located where the lumbosacral spine and the pelvis meet. When an SI joint is inflamed, patients will often feel that the hip is giving out. A SI joint injection is also both diagnostic and therapeutic. These injections temporarily eliminate pain by filling the SI joint with a medication that numbs the ligaments, joints, and joint capsule around the SI joint.
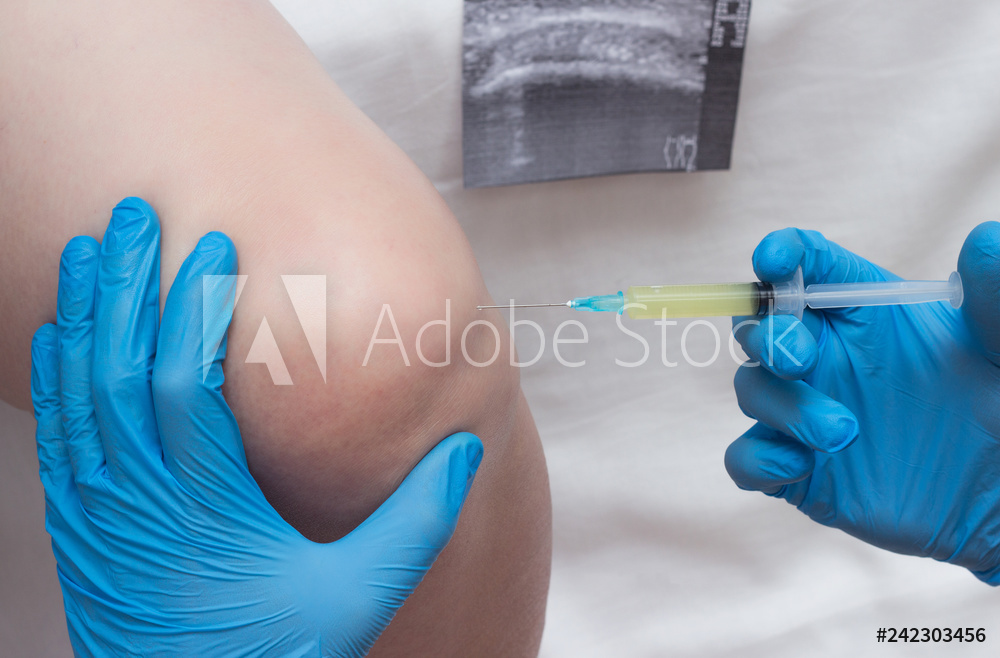
MINOR INJECTIONS
All of the injections we do at Agape are outpatient procedures, but these injections often don’t even require the use of our Fluoroscope. Instead, these minor injections can ordinarily be done using ultrasound to guide the needle.
Hip, Shoulder, & Knee Injections
Any joint can experience injury, arthritis, or mechanical stress, which may cause pain in the joint and the surrounding areas. For example, a hip joint injection can benefit patients with pain in the hip, low back, buttock, or leg; knee pain can radiate up and down the legs; shoulder pain can radiate into the neck. These joint injections involve injecting a steroid and an anesthetic agent directly into the joint using ultrasound guidance. The injection can help confirm diagnosis as well as relieve pain and discomfort in the joint.

Trigger Point Injections
A trigger point is a sensitive or irritable spot that can be a source of soft tissue pain. Trigger points are commonly found in muscle (myo) and its lining (fascia) and are called “myofascial” trigger points. The painful point can be felt as a nodule or band in the muscle, and a twitch response can be elicited on stimulation of the trigger point. Trigger points can result from strains, repetitive use injuries, stress, and muscle tension conditions. An anesthetic medication and sometimes an anti-inflammatory steroid is injected directly into the trigger point(s). These injections are done in the clinic. Trigger point injections have been found to be very effective in relieving pain. They are often used in combination with exercise, heat, cold, and medication.
MORE INTERVENTIONAL PROCEDURES
Kyphoplasty
Kyphoplasty is a minimally invasive procedure that will stabilize fractures of the body due to cancer, benign lesions, or osteoporosis. A balloon Kyphoplasty can restore the vertebral body height and reduce back pain. To gently elevate the fractured vertebrae, the doctors will use orthopedic balloons and to return them to the correct position. The now accessible cavity is then filled with bone cement, which will support the surrounding bone by creating an internal cast. In addition, studies have shown this procedure can provide rapid and sustained pain relief, improved mobility, enhanced quality of life, and lessened use of narcotic analgesics compared to non-surgical management.
Spinal Cord Stimulator
Spinal cord stimulation is a treatment for patients who suffer from chronic neuropathic (nerve) pain in the trunk and extremities. First, a temporary evaluation is performed where two leads with electrodes are inserted through a needle into the epidural space above the spinal cord. Next, an electrical block is programmed. The patient will try the temporary system for a week to assess their percentage of pain relief through their day-to-day activities. Every patient has a programmer that allows them to make changes to their programming during the week of their trial. Next, a temporary generator is placed in a bandage outside their body to power the leads during the trial. Leads are removed after one week, and pain relief is assessed.
A permanent implant is performed once a trial is complete and successful. This procedure is done in an ambulatory surgery center in the operating room as an outpatient. New leads are placed and connected to a generator that is implanted under the skin. The leads are programmed with a mild electrical block, and the patient receives a controller that allows them to make changes to their programming. Periodic reprogramming of the device in the office keeps the patient’s pain relief controlled.
